Insightec announced that France has introduced national reimbursement for unilateral magnetic resonance-guided focused ultrasound treatment for medication-refractory essential tremor, enabling hospitals across the country to offer the incisionless therapy using the Exablate Prime system. The reimbursement tariffs were published in the Journal Officiel of the French Republic following a positive clinical assessment from the Haute Autorité de Santé, creating a national funding pathway for hospitals to deliver the procedure to eligible patients.
Why France’s reimbursement decision signals growing regulatory confidence in focused ultrasound neurosurgery
The decision represents more than a pricing milestone. It signals that magnetic resonance-guided focused ultrasound is increasingly moving from experimental neurosurgical innovation toward mainstream clinical infrastructure in Europe. For companies developing device-based neuromodulation therapies, reimbursement decisions often determine whether a technology remains confined to specialized research centers or becomes a scalable treatment option. In this case, the French decision suggests regulators believe the clinical evidence supporting focused ultrasound has matured enough to justify national coverage for a defined patient population.
Essential tremor is widely recognized as the most common movement disorder globally, affecting millions of individuals and significantly impairing motor function, daily activity, and social participation. Although medications such as propranolol and primidone remain the first-line therapies, a substantial proportion of patients either fail to respond or cannot tolerate side effects. For these patients, surgical interventions have historically represented the next therapeutic step.
How MR-guided focused ultrasound is reshaping the treatment pathway for medication-refractory essential tremor
Deep brain stimulation has long been the dominant surgical treatment for severe essential tremor. The procedure involves implanting electrodes into the brain and connecting them to an implanted pulse generator that modulates abnormal neural circuits. While deep brain stimulation is clinically effective, it requires invasive surgery, implanted hardware, and ongoing device management.
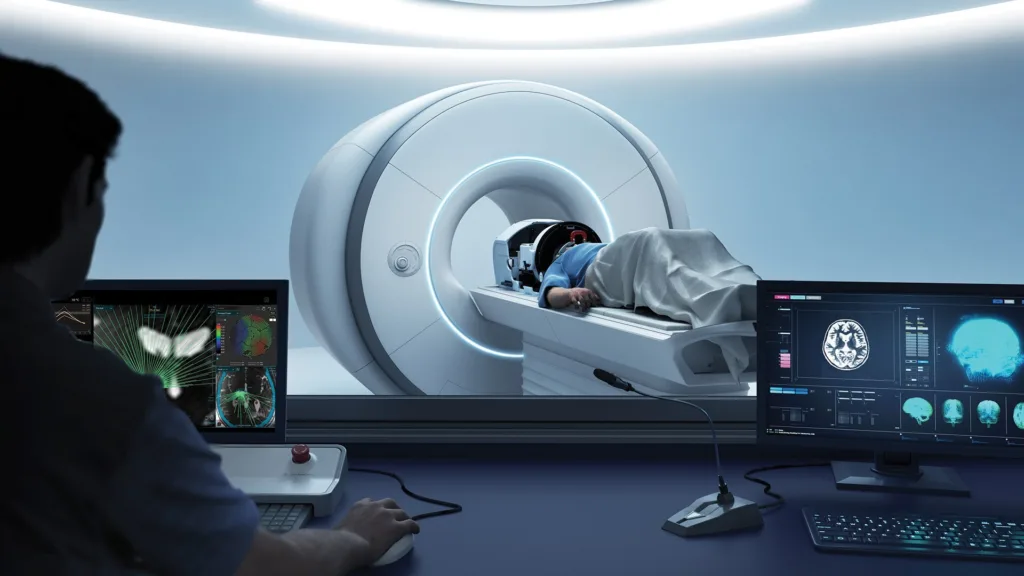
Magnetic resonance-guided focused ultrasound offers a fundamentally different therapeutic approach. Instead of implanting electrodes, the technology uses hundreds of converging ultrasound beams to create a precise thermal lesion in the thalamus, the brain region involved in tremor generation. Magnetic resonance imaging provides real-time guidance and thermometry, allowing physicians to visualize the target and monitor energy delivery during the procedure.
Because the treatment does not require incisions or implanted hardware, the procedure is often positioned as a less invasive neurosurgical alternative. Patients remain awake during treatment, and the therapy can be completed in a single session. Recovery times are typically shorter than those associated with implant-based neuromodulation procedures.
What this policy change reveals about the clinical evidence supporting incisionless neurosurgical therapies
The evidence base supporting magnetic resonance-guided focused ultrasound in essential tremor has expanded significantly over the past decade. Clinical trials have demonstrated improvements in tremor severity scores and functional disability, particularly in patients who have failed medication therapy. These studies have helped support regulatory approvals in several regions, including the United States and Europe.
However, adoption has historically been constrained by reimbursement uncertainty. Hospitals are unlikely to invest in specialized equipment without clear reimbursement frameworks, particularly for procedures involving advanced imaging integration and neurosurgical expertise. National coverage decisions therefore serve as powerful catalysts for diffusion of new medical technologies.
Why focused ultrasound is emerging as a competing alternative to deep brain stimulation in tremor care
In the French system, reimbursement decisions typically follow evaluation by the Haute Autorité de Santé, which assesses clinical benefit, comparative effectiveness, and cost-effectiveness before recommending national funding. The positive assessment for magnetic resonance-guided focused ultrasound effectively validated the therapy’s clinical value within the French healthcare system.
The publication of tariffs transforms that assessment into operational reality. Hospitals can now offer the procedure knowing that treatment costs will be reimbursed through the national Diagnosis Related Group system. This shift may encourage neurosurgical centers to invest in the necessary equipment and training.
From a technology perspective, Insightec’s Exablate platform sits at the center of this evolving treatment paradigm. The system integrates magnetic resonance imaging with ultrasound energy delivery, allowing clinicians to target specific brain structures with millimeter-level precision.
What France’s decision could mean for European adoption of image-guided neuromodulation technologies
Industry observers note that focused ultrasound has broader potential beyond movement disorders. Research programs are exploring applications ranging from psychiatric conditions to drug delivery across the blood-brain barrier. While many of these applications remain experimental, the expanding clinical footprint of focused ultrasound systems could accelerate research and development in related fields.
The French reimbursement decision may also influence regulatory thinking across other European healthcare systems. Reimbursement policies often evolve through a pattern of early adopters followed by broader regional alignment. When a large national system such as France establishes coverage for a new technology, neighboring countries frequently examine similar evidence and consider parallel policy decisions.
How hospital infrastructure and imaging integration will shape real-world adoption of focused ultrasound therapy
Nevertheless, several challenges remain before magnetic resonance-guided focused ultrasound becomes a standard treatment pathway for essential tremor across healthcare systems. One limitation is that the therapy is currently approved only for unilateral treatment in many jurisdictions, meaning the procedure targets tremor on one side of the body.
Another constraint involves patient selection. The therapy is primarily indicated for individuals who are medication-refractory and meet specific imaging and anatomical criteria. Not all patients are suitable candidates, and careful screening remains necessary to ensure safe outcomes.
Health system infrastructure also plays an important role. Magnetic resonance-guided focused ultrasound requires integration with high-field magnetic resonance imaging scanners and specialized neurosurgical teams. Hospitals without existing functional neurosurgery programs may face barriers to implementing the technology, even with reimbursement in place.
What clinical registries and long-term outcome tracking may reveal about durability of tremor control
Clinical registries mandated by French authorities may therefore play a critical role in shaping future policy decisions. By requiring hospitals to document patient outcomes and long-term results, regulators can gather real-world evidence about effectiveness, durability, and potential complications.
These data may influence future expansion of reimbursement criteria or adjustments to treatment guidelines. Long-term follow-up will be particularly important in determining whether focused ultrasound can maintain durable tremor control comparable to implant-based neuromodulation therapies.
What clinicians, regulators, and device manufacturers will watch next in focused ultrasound development
For Insightec, the French reimbursement decision reinforces the strategic importance of market access alongside regulatory approval. Even the most clinically promising technologies require reimbursement pathways to achieve meaningful patient reach.
The broader neuromodulation sector may also take note of the decision. Device companies developing non-invasive or minimally invasive neurological therapies are increasingly competing to demonstrate improved outcomes, reduced surgical burden, and favorable health economics.
Ultimately, the French policy change illustrates how the intersection of clinical evidence, regulatory evaluation, and reimbursement policy determines whether innovative medical technologies transition from experimental tools to routine clinical practice. As focused ultrasound systems continue to accumulate clinical data and real-world outcomes, additional healthcare systems may revisit their own reimbursement frameworks.