InventHelp disclosed the development of a patent-pending heat therapy device for hands and wrists, identified as TPL-346, based on an inventor-submitted concept intended to deliver targeted thermal relief for hand and wrist pain. The product, described as a heat therapy mitten, is positioned as a non-pharmacologic option aimed at reducing pain and swelling in users with chronic hand discomfort, but has not been linked to clinical testing, regulatory clearance, or defined medical indications.
Why this announcement matters more for the device ecosystem than for clinical practice today
While the disclosure itself is modest, it surfaces a recurring tension in the pain management and medical device landscape: the widening gap between consumer-oriented therapeutic products and the evidence standards required for clinical adoption. Heat therapy for musculoskeletal pain is not new. It is among the most established non-invasive modalities used for osteoarthritis, repetitive strain injuries, and nonspecific hand pain. What remains unresolved is not whether heat works, but whether incremental device design changes meaningfully alter outcomes, usability, or adherence in ways that justify regulatory or reimbursement consideration.
Industry observers note that products emerging through invention licensing platforms such as InventHelp often sit in an ambiguous zone. They are more sophisticated than consumer wellness accessories but fall short of regulated medical devices. This positioning can enable faster commercialization, but it also caps the ceiling for clinical credibility and payer interest.
What is genuinely new here versus what is incremental
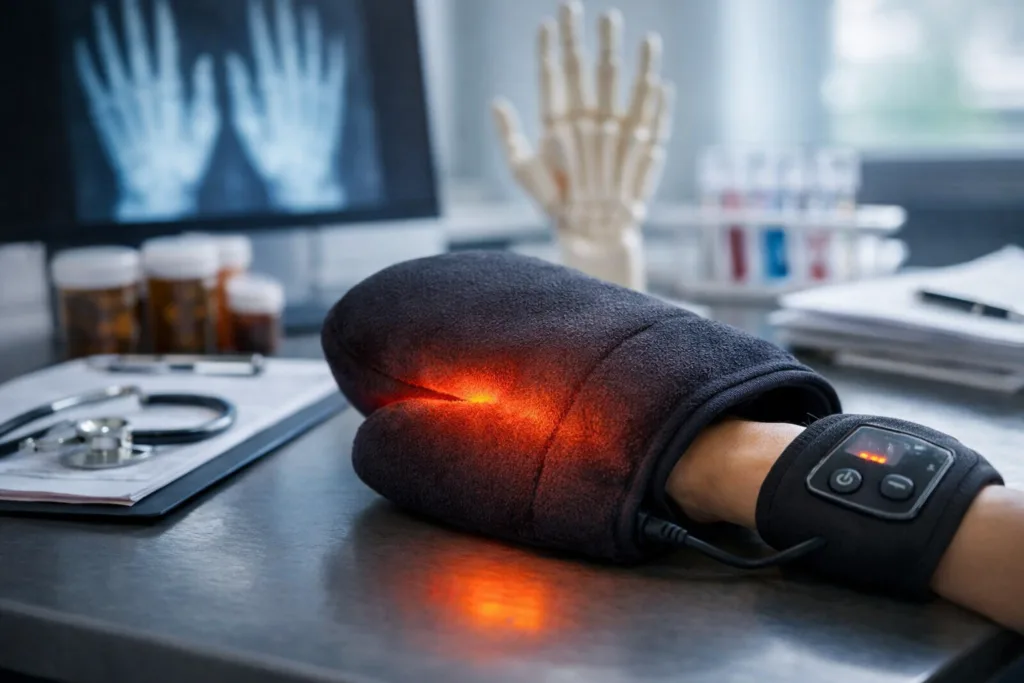
The heat therapy mitten does not introduce a novel therapeutic mechanism. Localized thermal application has decades of clinical and consumer use, supported primarily by symptom relief rather than disease modification. The novelty, if any, lies in the ergonomic and targeting claims, specifically the idea that a mitten-style enclosure could deliver more uniform or sustained heat to both hands and wrists compared with reusable gel packs, electric heating pads, or compressive wraps.
Clinicians tracking non-pharmacologic pain interventions tend to evaluate such products less on novelty and more on reproducibility and patient adherence. Without data on temperature control, duration consistency, or safety thresholds, the device remains functionally equivalent to existing heat delivery options already available at lower cost and broader scale.
Comparison with existing hand and wrist pain interventions
From a clinical perspective, heat therapy occupies a supportive role rather than a primary treatment pathway. For inflammatory arthritis, carpal tunnel syndrome, or post-traumatic stiffness, heat is typically adjunctive to splinting, physical therapy, or pharmacologic management. Numerous FDA-cleared devices already exist in this space, including electrically powered heating wraps and infrared-based systems, some with clinical labeling for temporary pain relief.
What differentiates regulated devices from consumer inventions is not the physical form factor, but the presence of safety testing, temperature regulation safeguards, and defined use conditions. Regulatory watchers suggest that without pursuing clearance as a Class I or Class II medical device, products like TPL-346 will remain limited to over-the-counter wellness positioning, regardless of anecdotal user benefit.
Clinical relevance and evidence limitations
The absence of any referenced clinical evaluation is the most consequential limitation. Even small observational studies demonstrating pain score reductions, grip strength improvement, or functional outcomes could materially shift how such a device is perceived by clinicians. In their absence, the product relies entirely on subjective claims that are common across hundreds of similar offerings.
From an evidence-based medicine standpoint, the device does not yet answer critical questions. These include whether targeted heat delivery improves outcomes beyond generic warming methods, whether prolonged use introduces skin or nerve risks, and whether certain patient populations benefit more than others.
Regulatory pathway ambiguity and its implications
InventHelp disclosures typically do not clarify regulatory intent, and this case is no exception. If positioned strictly as a consumer wellness product, the device avoids regulatory hurdles but forfeits clinical legitimacy. If the goal were medical device classification, even a low-risk pathway would require documented safety controls, labeling discipline, and post-market vigilance.
Regulatory observers note that many early-stage therapeutic inventions stall at this decision point. Pursuing clearance adds cost and time but unlocks clinician trust and institutional adoption. Avoiding it accelerates market entry but confines the product to direct-to-consumer channels with limited differentiation.
Adoption and reimbursement realities
From a reimbursement perspective, the device currently has no plausible pathway. Heat therapy accessories are rarely reimbursed unless bundled within broader physical therapy regimens or durable medical equipment categories with established codes. Even then, payers typically favor standardized, low-cost options.
This reality shapes the commercial ceiling. Without reimbursement, adoption depends on consumer willingness to pay out-of-pocket for incremental comfort rather than demonstrable clinical improvement. That model can support niche success but not scalable healthcare impact.
Manufacturing, scalability, and design control considerations
Another underexamined factor is manufacturing consistency. Heat-based devices require precise control over materials, insulation, and temperature retention to ensure safety and repeatability. For inventor-led products, scaling from prototype to mass production often introduces variability that undermines the original value proposition.
Industry veterans point out that many promising ergonomic designs lose effectiveness once production tolerances and cost constraints are introduced. Without transparency into manufacturing partners or quality systems, it is difficult to assess whether TPL-346 can maintain functional integrity at scale.
Risks, blind spots, and unresolved questions
The primary risk is commoditization. The market for hand and wrist heat therapy is already saturated, and differentiation without data is fragile. Another risk is consumer confusion, particularly if pain relief claims are interpreted as substitutes for medical evaluation or treatment.
Unresolved questions include whether the device offers adjustable or regulated heat, how long it maintains therapeutic temperature, and whether it accommodates bilateral or condition-specific use cases. These details matter far more to clinicians than broad comfort claims.
What clinicians, regulators, and industry observers are likely to watch next
For clinicians, the threshold is simple. Evidence. Even modest pilot data could shift perception. For regulators, clarity around intended use and claims will determine whether oversight becomes necessary. For industry observers, the key signal will be whether InventHelp positions the device toward licensing with an established medical device manufacturer or keeps it within consumer wellness channels.
Until then, the heat therapy mitten functions less as a breakthrough and more as a case study in how many pain management needs remain underserved by rigorously validated, accessible non-pharmacologic tools.