Bristol Myers Squibb and Pfizer have brought Eliquis, the oral anticoagulant apixaban, into a new direct access channel through Mark Cuban Cost Plus Drug Company, making the medicine available to cash-paying patients in the United States from April 27, 2026. The move places one of the country’s most widely prescribed branded blood thinners inside a transparent pharmacy model at a time when drug pricing pressure, Medicare negotiation, pharmacy benefit manager scrutiny, and patient affordability concerns are reshaping the commercial strategy of large pharmaceutical manufacturers.
Why direct-to-patient pharma access is no longer a fringe commercial experiment
The Eliquis launch on Cost Plus Drugs should not be read only as a discount pharmacy announcement. It is a signal that direct-to-patient pharma access is moving from the margins of drug distribution into the strategic toolkit of major branded manufacturers. For years, direct access models were mostly associated with low-cost generics, cash-pay telehealth, dermatology products, erectile dysfunction medicines, weight management services, or manufacturer patient assistance portals. Eliquis changes the optics because it is a major cardiovascular brand tied to serious chronic disease management and a large commercial franchise.
The shift matters because pharmaceutical companies are trying to solve several problems at once. They need to preserve access for patients facing high out-of-pocket costs, protect brand reputation in an environment hostile to opaque pricing, respond to policymakers demanding affordability, and reassure investors that mature blockbuster drugs can remain resilient even as pricing reform accelerates. Direct-to-patient platforms do not replace insurance, Medicare Part D, formulary negotiations, or pharmacy benefit managers. However, they create visible alternative routes that can reduce friction for specific patient groups and show that manufacturers are not entirely passive in the face of affordability criticism.
The unresolved question is whether these models can scale beyond selective use cases. A transparent cash price may help patients who are uninsured, underinsured, or exposed to high deductibles, but many prescriptions still move through employer plans, Medicare, Medicaid, commercial insurance, and pharmacy benefit manager-controlled formularies. Direct access can simplify one pathway, but it does not simplify the entire U.S. drug pricing system. That distinction will matter as more drugmakers consider whether direct-to-patient access is a genuine commercial channel or mainly a pressure-release valve.
How Eliquis gives the direct pharmacy model a much bigger credibility test
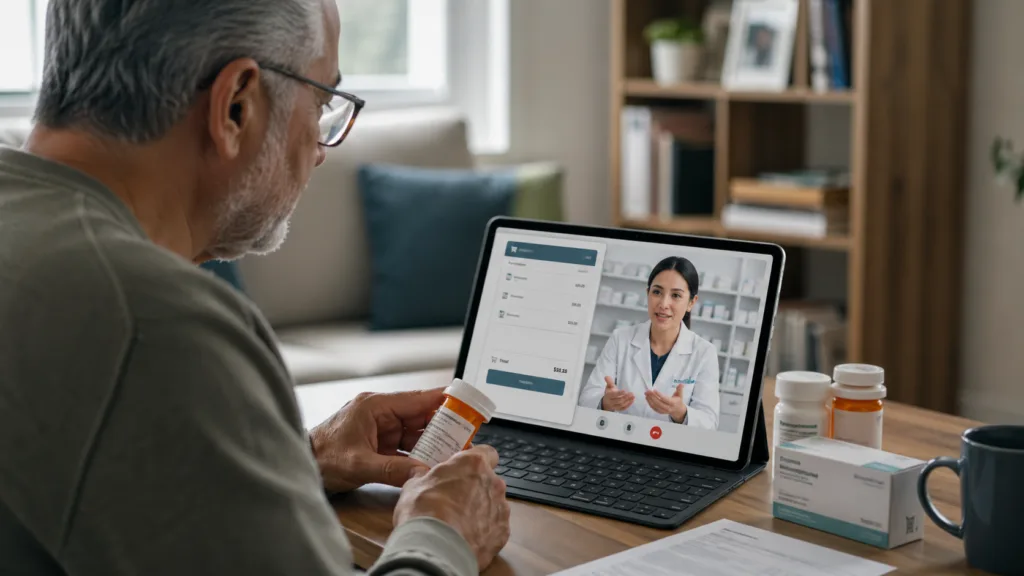
Eliquis is a particularly important test case because oral anticoagulants are not casual consumer products. Apixaban is used to reduce the risk of stroke and blood clots in adults with non-valvular atrial fibrillation, and to treat or reduce the recurrence risk of deep vein thrombosis and pulmonary embolism. These are high-consequence conditions where therapy interruption, affordability-related non-adherence, or confusion about access can carry serious clinical risk.
That clinical context gives the Cost Plus Drugs collaboration a sharper edge. A patient who cannot afford an anticoagulant may not simply delay a lifestyle medicine. They may face a higher risk of serious vascular events if treatment is stopped or missed without medical guidance. From a public health perspective, any access model that reduces abandonment or improves predictability can have value. From a commercial perspective, the same model can help manufacturers defend prescription continuity in a market where payer design and patient cost-sharing can weaken adherence.
However, the seriousness of the therapy also limits how far direct access can go. Eliquis still requires a prescription, appropriate clinical evaluation, safety monitoring, and patient understanding of bleeding risk. Direct-to-patient access may make the transaction clearer, but it does not convert anticoagulation into a simple e-commerce purchase. For clinicians and regulators, the key question will be whether convenience and affordability are paired with adequate clinical safeguards, especially when patients shift between insurance-based and cash-pay channels.
Why drugmakers are using direct access models as pricing pressure intensifies
The rise of direct-to-patient pharma access is happening because the old commercial model is under strain. Pharmaceutical manufacturers have long operated within a complex system involving list prices, rebates, wholesalers, pharmacies, pharmacy benefit managers, insurers, copay cards, patient assistance programmes, and government reimbursement. That system can work commercially, but it is increasingly difficult to defend publicly because patients often see only the final out-of-pocket cost, not the hidden rebate and contracting architecture behind it.
For branded drugmakers, that creates a reputational and policy problem. A medicine can be clinically valuable and still become politically vulnerable if patients associate it with unpredictable costs. The Inflation Reduction Act and Medicare drug price negotiation have made that vulnerability more concrete. Drugs with high Medicare spending and no immediate generic or biosimilar competition are now more exposed to negotiated pricing, public comparison, and future scrutiny.
Direct access models offer manufacturers a way to present a simpler affordability story. A defined cash price, a manufacturer-supported portal, or a transparent online pharmacy route is easier to explain than a rebate-driven system. It also gives companies more control over the patient-facing narrative. The risk is that these initiatives may be seen as selective fixes rather than structural answers. If direct access remains limited to certain patients, certain drugs, or certain price points, critics may argue that the broader system remains fundamentally unchanged.
How Cost Plus Drugs, LillyDirect, and PfizerForAll point to different versions of the same trend
The current direct-to-patient landscape is not one model. It is a collection of overlapping experiments. Cost Plus Drugs is built around transparent pharmacy pricing and direct online access. LillyDirect connects patients with independent telehealth providers and pharmacy fulfillment services for selected Eli Lilly and Company medicines. PfizerForAll is positioned as a digital access and support platform for Pfizer therapies. Amazon Pharmacy and Amazon One Medical are also pushing into prescription access, chronic care coordination, and medication delivery, particularly in high-demand areas such as weight management.
These models differ in ownership, clinical integration, therapeutic focus, and commercial intent. Some are manufacturer-led. Some are platform-led. Some emphasize cash pricing. Others emphasize navigation, telehealth, insurance support, or fulfillment. The common thread is that the patient relationship is becoming more strategically important. Drugmakers no longer want their role to end at manufacturing and payer negotiation. They increasingly want a visible channel through which patients can understand, access, and remain on therapy.
The opportunity is significant, but so is the complexity. Direct-to-patient pharma access requires careful handling of compliance, prescribing independence, advertising rules, data privacy, clinical oversight, adverse event reporting, and reimbursement boundaries. A model that works for a migraine medicine or an obesity drug may not translate easily to oncology, immunology, cardiology, or rare disease. The sector is moving toward direct access, but it is not moving toward a single universal template.
Why pharmacy benefit managers remain central to the direct access debate
The growth of direct-to-patient access also reflects rising scrutiny of pharmacy benefit managers. PBMs occupy a powerful position in the U.S. prescription drug system because they influence formulary placement, rebate structures, pharmacy networks, and patient cost-sharing. Manufacturers may dislike PBM leverage, but they still depend on payer access to reach large patient populations. That is why direct-to-patient models are best understood as parallel channels rather than outright replacements.
For patients, the appeal of direct access is clarity. Instead of navigating copays, prior authorization, deductible surprises, and pharmacy counter uncertainty, a patient may be able to see a defined price or a clearer access route. For manufacturers, the appeal is partly strategic. A direct channel gives them a way to reach patients who are poorly served by the insurance-based pathway, while also demonstrating responsiveness to affordability concerns.
The limitation is that PBMs will not be displaced easily. Employer plans, Medicare Part D plans, and commercial insurers still rely on PBMs for drug benefit management. Many patients will continue to receive better pricing through insurance than through cash-pay options, depending on their plan design. Direct access may therefore pressure the system at the margins, but it is unlikely to replace the dominant reimbursement structure in the near term. The more realistic outcome is a hybrid market where insured access, manufacturer portals, transparent cash-pay pharmacies, and digital care platforms coexist.
How direct-to-patient access could reshape blockbuster lifecycle management
For mature branded drugs, direct-to-patient access may become part of lifecycle management. Traditionally, companies defended blockbuster franchises through new indications, formulation improvements, real-world evidence, payer contracting, patient support, and brand loyalty. Direct access adds another layer by helping manufacturers retain patients who might otherwise abandon therapy because of cost or friction.
Eliquis fits this logic well. Bristol Myers Squibb and Pfizer are managing a medicine with major clinical relevance, large revenue importance, and long-term exposure to policy and competition risks. A transparent pharmacy partnership does not eliminate those risks, but it strengthens the access narrative at a sensitive time. It also signals that the manufacturers are willing to experiment with channels that may have once seemed more aligned with disruptors than with large pharmaceutical companies.
The strategic risk is that direct access can reveal uncomfortable price comparisons. Once a cash price is visible, patients, payers, policymakers, and investors may compare it with list prices, negotiated prices, international prices, and future generic prices. Transparency can build trust, but it can also sharpen scrutiny. Manufacturers entering this space must be prepared for both effects.
Why investors should pay attention to direct-to-patient pharma models
For investors, direct-to-patient pharma access is not yet a primary valuation driver for most large pharmaceutical companies. Pipeline productivity, patent cliffs, regulatory approvals, earnings growth, capital allocation, and merger activity still matter more. However, access strategy is becoming more relevant because pricing pressure now affects revenue durability, political risk, and brand resilience.
Bristol Myers Squibb and Pfizer illustrate the point. Both companies have mature commercial portfolios and are under investor pressure to show that they can protect cash flow while building or rebuilding growth engines. Eliquis remains important to that equation. Any strategy that supports patient continuity, reduces access friction, or improves the public affordability narrative may help defend the franchise, even if it does not dramatically change near-term revenue forecasts.
The same logic applies across the sector. Eli Lilly and Company, Novo Nordisk A/S, AstraZeneca PLC, Amgen Inc., Johnson & Johnson, and other major drugmakers are all navigating a market where patients expect digital access, policymakers expect affordability, and investors expect margin discipline. Direct-to-patient channels sit at the intersection of those expectations. They are unlikely to solve every pricing problem, but they may become an increasingly visible part of how drugmakers manage market risk.
What regulators, clinicians, and industry observers will watch next
The next question is whether direct-to-patient pharma models remain concentrated in a few high-profile categories or expand across chronic disease, specialty medicine, and complex care. If more branded drugs move into transparent cash-pay or manufacturer-linked digital access channels, the U.S. market could shift toward a more fragmented but more patient-visible access system. That may benefit some patients, but it could also create confusion if different channels offer different prices, eligibility rules, and support structures.
Regulators will likely watch how these models handle safety, prescribing independence, promotional boundaries, and patient data. Clinicians will watch whether patients understand when to use direct access and when to stay within coordinated care pathways. Payers and PBMs will watch whether manufacturer-backed channels undermine formulary control or simply serve patients who were already outside the covered system. Investors will watch whether these initiatives protect revenue, improve adherence, or mainly generate public relations value.
The direction of travel is already clear. Direct-to-patient pharma access is becoming harder for the industry to ignore. The Eliquis-Cost Plus Drugs collaboration shows that even large, established, heavily prescribed branded medicines can be placed inside more transparent access models. That does not mean the pharmaceutical supply chain is about to be overturned. It does mean the patient-facing side of drug commercialization is becoming a more important competitive frontier.
Why direct-to-patient access may become pharma’s next serious commercial defence
The Eliquis move should be treated as an early marker of a broader commercial shift. Direct-to-patient pharma access is not replacing the traditional payer system, and it is not a magic cure for high drug prices. However, it gives branded manufacturers a new way to defend access, protect reputation, and respond to patients who are tired of not knowing what their medicines will cost until the system has already confused them.
The winners will not simply be the companies that launch the flashiest patient portals. The winners will be the manufacturers that can combine transparent access with clinical credibility, payer discipline, safety oversight, and genuine affordability. Direct-to-patient pharma is entering its serious phase now. The Eliquis launch shows that the model is no longer just about disruption from outside the industry. Big pharma is starting to use the same playbook, and that is when a trend usually stops being cute and starts becoming structural.