Royal Philips has announced the launch of Verida, its next-generation spectral computed tomography (CT) system powered by fully embedded artificial intelligence. Unveiled at RSNA 2025, Verida is the first detector-based spectral CT to integrate AI across the imaging chain, from acquisition to reconstruction. The system is CE-marked and pending 510(k) clearance in the United States, with select market availability expected in 2026. Philips is positioning the platform as a clinical-ready alternative to photon-counting CT, offering faster scans, lower radiation doses, and improved diagnostic confidence, particularly in high-throughput environments like cardiac imaging.
Why AI-native integration could change expectations for spectral CT
Philips’ core differentiator with Verida is the full-stack integration of artificial intelligence within a detector-based spectral architecture. This marks a departure from traditional CT systems that either apply AI post-reconstruction or rely on standalone modules to augment image quality. In Verida, AI is foundational to every stage, starting with noise suppression during acquisition and continuing through real-time spectral image reconstruction.
According to industry analysts, this system-level approach could give Philips a strategic advantage in the growing segment of AI-native radiology tools, where the emphasis is shifting from experimental utility to operational scalability. As hospital systems prioritize speed, throughput, and image consistency over speculative technology upgrades, Verida’s focus on embedded intelligence offers a path toward broader adoption without requiring a complete technology overhaul.
What this reveals about Philips’ challenge to photon-counting CT
By positioning Verida as an evolution of its well-established spectral CT ecosystem, Royal Philips is also implicitly drawing a line against photon-counting CT systems, which have captured attention but remain limited in clinical penetration. While photon-counting CT is often described as the next frontier in diagnostic imaging, it still faces challenges in workflow integration, cost, and data processing requirements.
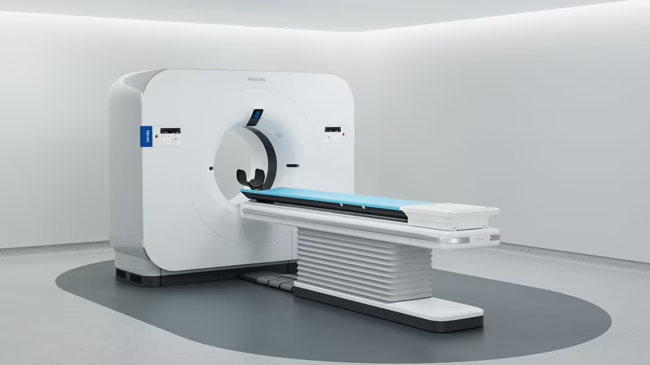
Philips, by contrast, has opted to extend its proprietary dual-layer detector platform, which has seen global deployment in more than 800 clinical settings. Verida leverages the company’s third-generation Nano-panel Precise detector, tuned for noise reduction and AI optimization. This continuity allows Philips to claim technological maturity and backwards compatibility, while still offering step-change improvements in performance through deep learning-enhanced spectral imaging.
The company argues that Verida’s clinical outcomes are already comparable to those promised by photon-counting systems, with the added benefit of lower total cost of ownership and seamless compatibility with picture archiving and communication systems (PACS).
How Verida accelerates cardiac imaging and workflow reliability
While Verida can be deployed across general CT applications, its early endorsements point toward cardiovascular imaging as a strategic clinical entry point. Professor Eliseo Vañó Galván, a cardiovascular radiologist and department chair at Hospital Nuestra Señora del Rosario in Madrid, noted that Verida’s spectral fidelity and workflow simplicity could make spectral imaging routine for all cardiac CTs.
The ability to generate comprehensive spectral data in a single scan without scan-time tradeoffs is particularly relevant in cardiology, where speed, motion handling, and lesion visibility under contrast conditions are critical. The claim that Verida can reconstruct 145 images per second and deliver full exams in under 30 seconds introduces not only a clinical advantage but also a potential operational shift. For high-volume centers, this enables up to 270 exams per day, doubling current expectations and reducing delays that strain diagnostic workflows.
Clinicians tracking cardiac imaging trends may view Verida’s dose reduction capabilities as another compelling feature. With radiation exposure remaining a concern, especially for repeat cardiac scans or younger patients, Verida’s AI-optimized acquisition protocols and dose efficiency claims could support adoption in risk-sensitive clinical pathways.
Why workflow compatibility may drive faster adoption
A key barrier to adoption for emerging CT technologies has been the need to retrain staff, alter workflows, or manage complex new interfaces. Verida sidesteps these pitfalls by embedding its spectral and AI functions into a software-defined architecture that builds directly on existing Philips installations. For hospital systems already running Philips spectral CT platforms, Verida offers a natural upgrade path rather than a disruptive replacement cycle.
This is particularly important in regions where imaging departments are facing both staffing shortages and budgetary constraints. Verida’s potential to cut repeat scans and reduce interpretation variability means it may not only deliver better imaging, but also reduce the burden on overextended radiology teams. This operational framing could be as influential as the clinical performance in procurement decisions.
From an environmental perspective, Philips claims Verida reduces energy consumption by up to 45 percent compared to conventional CT systems, which may add to its appeal in regions adopting green hospital standards.
What regulators and payers may scrutinize next
Despite strong positioning, Verida’s performance claims will require validation across broader populations before reimbursement frameworks adjust accordingly. Regulators may seek comparative evidence not only against legacy CT modalities but also against emerging photon-counting systems now undergoing clinical evaluation.
Questions may also be raised about the system’s generalizability across less standardized imaging contexts, including oncology or emergency trauma, where spectral information may require additional interpretive layers or AI training datasets.
The 510(k) process in the United States, while typically straightforward for imaging hardware extensions, could become more complex given Verida’s embedded AI framework. Regulators have become increasingly cautious in evaluating AI-native platforms that may evolve over time through software updates. While this offers future flexibility, it also raises concerns about maintaining predictable performance, especially in high-stakes imaging environments.
What this implies for platform longevity and upgrade cycles
By treating AI as part of the system’s core architecture, Philips is reinforcing its software-defined strategy across diagnostic imaging. This approach aligns with a broader industry shift where platform value increasingly comes from algorithms rather than hardware replacement. If Verida’s architecture proves stable, it may allow Philips to release iterative AI updates that improve performance without forcing costly hardware swaps.
That said, enterprise imaging teams may want to assess whether Verida’s performance scales consistently across diverse patient groups and whether the AI models used in reconstruction are robust against edge cases, such as rare diseases or imaging artifacts from implants or prior interventions.
Competitive dynamics and strategic signaling
Verida’s launch at RSNA 2025 is also a calculated signal to the broader market that Philips is not ceding the AI narrative to newer entrants or photon-counting specialists. It is asserting leadership not by betting on unproven sensor technology but by deepening the capability of an existing spectral platform.
Competitors with photon-counting ambitions may now be under pressure to fast-track clinical validation or demonstrate equivalent workflow reliability. At the same time, providers evaluating long-term imaging investments may now consider whether waiting for photon-counting maturity is justified, or whether a proven, AI-enhanced spectral platform like Verida meets clinical needs today.
In this context, Verida is not merely a product launch—it is a strategic line in the sand, suggesting that imaging innovation in 2026 will be as much about seamless integration and AI scalability as about hardware novelty.
Conclusion: From research edge case to clinical backbone?
If Philips can translate Verida’s claims into consistent, real-world performance, the platform may do more than solidify spectral CT’s value—it could push spectral imaging into the mainstream across multiple specialties. The system’s fast reconstruction speeds, low-dose protocols, and AI-native design position it as more than a clinical tool. It is an infrastructure investment aligned with the future of radiology.
The next inflection point will likely come with post-clearance adoption data and head-to-head performance studies. Until then, Verida sets a high bar for what AI in CT imaging must deliver—both in pixels and in productivity.