Soin Neuroscience and BIOTRONIK Neuro have announced a research collaboration focused on evaluating novel waveform technology and adaptive spinal cord stimulation programming aimed at enhancing chronic pain treatment outcomes. The partnership integrates proprietary signal tuning algorithms from Soin Neuroscience with the programmable Prospera SCS system developed by BIOTRONIK Neuro, reinforcing a broader industry shift toward patient-specific neuromodulation.
What this collaboration reveals about the next evolution in spinal cord stimulation
Spinal cord stimulation has long been recognized as a viable therapeutic option for chronic pain, particularly when conservative interventions fail or opioid use is contraindicated. However, variability in patient response remains a central challenge. For years, device manufacturers and clinicians have sought more consistent, longer-lasting relief by refining waveform characteristics, adjusting pulse widths, and experimenting with paresthesia-free paradigms. This latest partnership attempts to go further by introducing real-time adaptability to the way stimulation is delivered.
At the heart of Soin Neuroscience’s contribution is a suite of investigational waveforms and adaptive algorithms designed to fine-tune stimulation parameters based on observed patient responses. This approach moves beyond static programming models that are often based on trial-and-error adjustments during clinical visits. Instead, it aims to personalize therapy dynamically, aligning stimulation delivery more closely with each patient’s specific needs and physiological feedback.
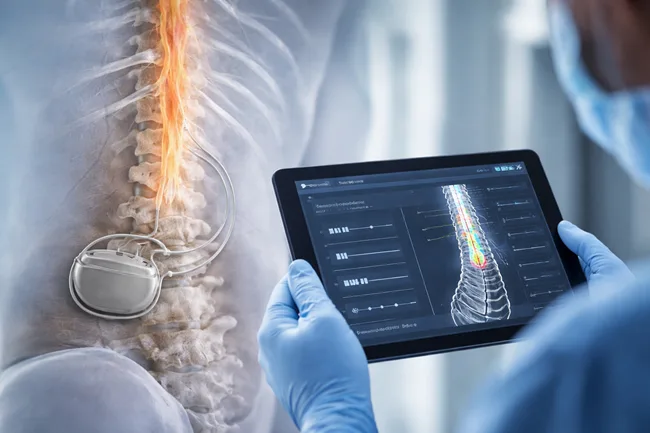
BIOTRONIK Neuro’s Prospera platform, built around its BioArc stimulation engine, provides the technical architecture to support these ambitions. The system allows for remote programming and expanded flexibility, making it capable of running novel waveform sequences without requiring device reinsertion or cumbersome in-clinic modifications. For both companies, the collaboration creates an opportunity to test whether combining adaptive logic with flexible hardware can improve therapeutic outcomes across a broader population of chronic pain patients.
Why precision waveform tuning could be the tipping point for neuromodulation
The SCS market has matured considerably over the past decade, but clinical differentiation remains a moving target. Manufacturers have attempted to distinguish their systems through smaller device footprints, rechargeable versus recharge-free options, expanded MRI compatibility, and increased battery longevity. However, many of these innovations have plateaued in terms of clinical impact.
Industry observers suggest that waveform customization could represent the next leap forward. Rather than delivering uniform signals across different pain conditions and anatomical targets, next-generation systems are experimenting with modulation that varies in intensity, frequency, and pattern based on feedback from the patient’s nervous system. This aligns with a broader movement in medtech toward smarter, more responsive therapeutics—where devices behave more like algorithms than static tools.
Clinicians tracking these developments are especially interested in how Soin Neuroscience’s adaptive algorithms will define and quantify “response.” If the system can accurately detect when a patient is under- or overstimulated, and then automatically adjust therapy within clinically accepted boundaries, it could reduce the trial-and-error burden typically borne by both physicians and patients. That, in turn, could accelerate time to therapeutic benefit and improve long-term adherence.
What remains unproven despite the technical promise
While the ambition behind this collaboration is significant, the underlying technology remains investigational. Soin Neuroscience’s algorithms and waveforms have not yet been validated in large-scale clinical studies, and no randomized trial data has been presented to compare their efficacy against current commercial standards. Without such evidence, the claims of improved personalization remain theoretical.
There is also the question of regulatory classification. Adaptive stimulation algorithms that modify therapy delivery in response to physiological signals may fall under emerging regulatory scrutiny around software as a medical device. Regulatory watchers note that clear guidance on algorithm transparency, safety thresholds, and override capabilities will be needed before such systems can be widely commercialized.
From a technical standpoint, real-time feedback mechanisms require a combination of high-fidelity signal detection, secure data processing, and low-latency transmission. These features must be integrated without compromising the battery life, safety, or reliability of the implantable hardware. Although BIOTRONIK Neuro’s Prospera platform is designed with modularity in mind, the integration of adaptive waveforms may require firmware upgrades, additional clinician training, or even updates to payer reimbursement models.
Scalability is another unknown. Early success in a controlled research setting may not translate into broader adoption if the technology proves complex to implement or difficult to personalize for patients with comorbid conditions, altered pain pathways, or previous SCS implant experience.
What clinicians and regulators will monitor going forward
The collaboration between Soin Neuroscience and BIOTRONIK Neuro is expected to draw close attention from several stakeholder groups. Clinicians are likely to focus on measurable improvements in responder rates, therapy durability, and reduction in reprogramming visits. These outcomes are particularly relevant in the context of rising healthcare costs and increased demand for outpatient efficiency.
For regulators, the emphasis will be on how personalization is achieved and whether adaptive programming introduces new safety considerations. Devices that autonomously adjust stimulation based on patient input or sensed signals must demonstrate that such changes do not create unintended consequences, such as nerve desensitization or overlapping stimulation fields. The software decision-making logic must also be explainable and auditable, particularly in light of evolving requirements around medical AI.
Payers will be looking for evidence that personalization results in fewer reoperations, reduced opioid usage, and improved quality of life metrics—outcomes that can justify premium device pricing or value-based reimbursement models.
If the collaboration can generate compelling early data, industry analysts believe the pathway to larger feasibility or pivotal trials could open quickly. Depending on the timing and structure of those studies, it may also influence how other neuromodulation firms prioritize adaptive algorithms and real-time feedback in their product pipelines.
Why this could signal a broader pivot in neuromodulation strategy
The Soin–BIOTRONIK collaboration is part of a broader rethinking of how neuromodulation technologies should evolve. The historical focus on hardware miniaturization and lead placement precision is gradually giving way to a software-centric vision. In this model, the value of the device lies not just in its form factor or battery capacity but in its intelligence—its ability to tailor therapy based on inputs, context, and patient response.
This mirrors changes happening in adjacent medtech segments such as cardiac rhythm management, deep brain stimulation, and sacral neuromodulation, where smart algorithms are increasingly used to guide therapy parameters. It also raises the possibility of longitudinal data collection, where SCS systems could someday contribute to broader pain registries or personalized treatment maps based on patient subtype and response history.
Whether this collaboration results in a commercial breakthrough or simply serves as a proof of concept, it sends a clear signal to the market: the next era of spinal cord stimulation will not be defined solely by what the device delivers, but by how intelligently and responsively it delivers it.